📖 Why I Wrote This Book
I began writing Cervicogenic Dizziness Relief after someone left a comment on one of my YouTube videos suggesting I “pin a book.” At the time, I had already spent years helping patients recover from cervicogenic dizziness and headaches, but I realized many people outside my clinic were still confused, misdiagnosed, or told their symptoms were “normal.”
This book was created to provide clear, structured guidance for people who want to understand what’s actually happening in their neck — and what to do about it safely and effectively.
Below, you can read the first several pages and see how the book approaches cervicogenic dizziness differently.
Table of Contents
Acknowledgements ………………………………………………………. iii
Foreword ……………………………………………………………………….v
Preface: The Inevitable Discovery ……………………………………vii
Introduction ……………………………………………………………………ix
- You Can Stop Cervical Dizziness and Neck Pain …………………………………………………………………………. 1
- How Your Neck Works and Why It Hurts ………………………………………………………………………… 8
- Common Causes of Neck Pain ………………………………………………………………………… 22
- How Neck Pain Causes Dizziness and Imbalance ………………………………………………………………………… 50
- How Do I Know If I Have Cervicogenic Dizziness? ………………………………………………………………………… 58
- Other Common Causes of Dizziness ………………………………………………………………………… 74
- Exercises to Relieve Neck Pain ………………………………………………………………………… 90
- Retraining Balance and Body Awareness ……………………………………………………………………….. 112
- Manual Therapy to Relieve Cervicogenic Dizziness ……………………………………………………………………….. 131
- When to Do Therapeutic Exercises ………………………………………………………………………… 146
- Instructions for People with Severe Dizziness ………………………………………………………………………….158
- Next Steps………………………………………………………169
- Closing Thoughts………………………………………………………171
- References………………………………………………………172
CHAPTER 1
YOU CAN STOP CERVICOGENIC DIZZINESS AND NECK PAIN
Introduction
I am not the first person to recognize that a problem with your neck can easily turn into an issue with dizziness and imbalance. In 1955, two doctors, Ryan and Cope, discovered that injecting their own necks with anesthetic drugs induced dizziness and imbalance. They called this newly discovered dizziness cervical vertigo. Since that time, this form of dizziness has been given a newer name: cervicogenic dizziness. After decades of clinical practice, I am now convinced that this form of dizziness is legitimate and occurs much more often than initially suspected. More importantly, I am pleased to report that, in most cases, cervicogenic dizziness can be alleviated with proper treatment.
I have found that gentle orthopedic manual therapy and specialized exercises can effectively alleviate cervical dizziness and neck pain. Medical research has verified these methods. Of all these interventions, I rapidly realized that specific stabilization exercises are often the key to achieving long-lasting relief from cervicogenic dizziness. These exercises can easily be learned and performed at home for effective self-treatment.
Over the last two decades, I have continuously refined the treatment of cervicogenic dizziness and neck pain. Specifically, I have identified a combination of gentle manual therapy and neck stabilization exercises for treating cervical dizziness. These exercises improve the neuromuscular control and strength of the neck and shoulder girdles. This approach also includes an essential postural correction exercise. Clinical research indicates that cervicogenic dizziness can be effectively treated through targeted therapeutic interventions. A recent systematic review and meta-analysis confirmed that manual therapy and exercise are beneficial in managing this condition (De Vestel et al., 2022).
The main features of the neck (cervical spine) include the bony vertebrae, discs, nerves, and the important muscles that support the spine against gravity. Pain in the neck will reflexively weaken the deep support muscles, allowing for repeated impingement and “pinching” of the neck joints. When the upper neck becomes the primary source of pain, common symptoms that may occur include headaches, dizziness, vertigo, TMJ pain, sinus pain, and discomfort around one or both eyes.
The exercises in this book are designed to restore the neck’s natural protective mechanisms. As the deep muscles regain their strength, pain and dizziness lessen, and good days begin to outnumber the bad days. Excitingly, many people notice improvement within days of starting the program.
The exercises only take a few minutes to perform and are usually recommended to be done twice a day. Hourly postural exercises are also included to prevent strain on the neck and reduce dizziness. This type of exercise fits nicely into a busy workday and can easily be accomplished at your desk. By investing just a few minutes a day, you can start to make positive changes and take back control of your quality of life.
To remain dizzy-free, readers will need to adopt good neck and back posturing during their day (especially during phone and computer use).
The Problem
It’s estimated that around 20-30% of people will experience dizziness at some point in their lives. In specific age groups, especially among older adults, the prevalence can be even higher. Studies suggest that nearly 30-50% of older adults report experiencing dizziness or balance issues, often linked to conditions like vestibular disorders, medications, or age-related changes.
Dizziness is one of the top 10 reasons why a person will visit their doctor. It can account for a significant portion of visits to specialists, such as neurologists and otolaryngologists. In primary care settings, dizziness might be a reason for consultation in about 5-10% of all visits. This can vary based on demographics, such as age. Possible reasons for their increased risk could be related to balance disorders, medication side effects, and advanced degeneration of the neck.
Cervicogenic dizziness, which originates in the cervical spine, is often described as less common than other causes of dizziness. Conservative estimates suggest it accounts for about 15–20% of all cases, particularly in people with whiplash or other neck problems.
However, more recent studies suggest the prevalence may be much higher. A large clinical observation of 1,000 patients reported that cervicogenic dizziness accounted for nearly 89% of all dizziness and vertigo cases. Other surveys have found that cervical spondylosis is a frequent cause of dizziness in older adults, that 20–90% of patients with whiplash report dizziness, and that nearly half of those with chronic neck pain experience cervicogenic dizziness (Li, Yang, Dai, & Peng, 2022). These wide-ranging figures highlight both the diagnostic challenges and the ongoing controversy surrounding this condition. Regardless of the exact percentage, what is clear is that cervicogenic dizziness is under-recognized and deserves far more clinical attention.
To fully appreciate why cervicogenic dizziness deserves greater attention, it’s important to look beyond the clinic and consider the broader
consequences it has on health, safety, and mental well-being.
Dizziness can pose a serious problem in society for many different reasons:
- Health Impact: Dizziness can signal underlying health problems, affecting individuals’ ability to work, drive, or perform daily activities. This can lead to increased healthcare costs and loss of productivity.
- Safety Risks: Individuals who experience dizziness are at a higher risk of falls and accidents, which can result in serious injuries. This is especially concerning for older adults, who may already face mobility challenges.
- Mental Health: Chronic dizziness can lead to anxiety and depression, as individuals may fear future episodes or feel isolated due to their condition.
- Social Stigma: Individuals who experience dizziness may struggle to communicate their experiences, leading to misunderstandings or a lack of support from others.
- Impact on Relationships: Dizziness can affect personal relationships, as individuals may avoid social situations or be perceived as unreliable if they frequently need to cancel plans due to dizziness.
Dealing with a dizziness disorder can alter your life dramatically in a negative way. Not only does it affect you physically, emotionally, and socially, but the need for ongoing, extensive treatment can be very costly. The treatment cost can vary widely based on several factors, including the underlying cause, type of treatment, and location. Here are some general estimates in the United States:
- Initial Consultation: A visit to a primary care physician can range from $100 to $300, while a specialist (like a neurologist or ENT) may charge between $200 and $500.
- Diagnostic Tests: Tests such as MRI or CT scans can cost between $500 and $3,000, while balance tests (like vestibular testing) may range from $300 to $1,000.
- Physical Therapy: Vestibular rehabilitation therapy sessions typically cost between $75 and $150 per session. A full course may involve multiple sessions. Moreover, if you are suffering from undiagnosed cervicogenic dizziness, this can often make your symptoms worse.
- Medications: Prescription medications for dizziness or underlying conditions can vary widely in cost, often ranging from $10 to $100 per month, depending on insurance coverage.
Overall, total treatment costs for dizziness can range from a few hundred to several thousand dollars, depending on the condition’s complexity and duration. Many of my patients have spent thousands of dollars visiting multiple doctors and vestibular therapists, only to find that their dizziness was not much better despite their exhaustive efforts. This highlights the importance of receiving a proper diagnosis and recognizing when neck dysfunction could lead to persistent dizziness. Despite the many problems that dizziness and neck pain pose, you can eliminate or greatly reduce your symptoms with the proper knowledge, exercises, and insight presented in the following chapters.
The Solution
You can stop your own cervicogenic dizziness. You may have thought that your options were limited to:
- Visiting a doctor.
- Visiting a chiropractor.
- Visiting a physical therapist.
- Taking medications.
- Having neck surgery.
- Some combinations of the above.
- Just living with your problem.
However, there is another solution. You can take charge of your own neck pain and dizziness. Through the exercises and manual therapy treatments outlined in this book, you can effectively eliminate or significantly reduce your cervicogenic dizziness.
In 2002, a landmark study from the University of Queensland, Australia, demonstrated that manipulative therapy combined with specific motor control exercises is effective in managing cervicogenic headache and neck pain (Jull et al., 2002). Moreover, this same research indicated that these positive outcomes were maintained in the long term. For over two decades, I have combined the previously mentioned exercises with gentle manual therapy, balance exercises, and exercises that prevent dizziness and improve eye-head coordination, using them as an effective treatment for cervicogenic dizziness. The heart of the method is to improve neuromuscular control and spinal stability of the neck to lessen your symptoms. For most of my patients, a combination of 3-4 exercises, performed once or twice daily, was sufficient to alleviate neck pain and dizziness.
The other significant contribution of the method is the importance of maintaining good sitting and standing posture. Proper spinal posture activates the deep muscle system of the neck and reduces stress on sore neck joints. Changing positions frequently and limiting time spent in sitting or lying down postures is equally essential for recovering from neck pain and dizziness. In this book, I will suggest postural exercises that you can perform at home or at work to help alleviate or reduce neck pain and dizziness.
Conclusion
The primary objective of this book is to teach you, the reader, how to manage your own cervicogenic dizziness effectively.
First, I will explain why cervicogenic dizziness occurs, and then I will suggest ways to avoid it during your day. I will teach you methods to manage your current symptoms and how to care for your condition if it reoccurs. Self-treatment of spinal conditions such as neck and back pain is now widely recommended as a first-line treatment option. Remember, only you can really help yourself in a true case of cervicogenic dizziness. However, I do still recommend that my patients work with other healthcare providers to rule out more serious conditions.
CHAPTER 5: How Do I Know If I Have Cervicogenic Dizziness
Introduction
Cervicogenic dizziness is a condition where dizziness arises from issues in the neck, typically due to musculoskeletal or neurological dysfunction. It can be challenging to differentiate this type of dizziness from other causes, such as vestibular disorders or inner ear problems, but understanding its unique characteristics can guide you toward proper diagnosis and treatment.
This chapter delves into the origins, diagnosis, and distinguishing features of cervicogenic dizziness, offering insights into its history, symptoms, and the various factors contributing to its development. Since the symptoms often overlap with other conditions, many patients go through lengthy evaluations before receiving an accurate diagnosis. Recognizing the signs of cervicogenic dizziness early can help you seek the right care and prevent unnecessary frustration or delays in treatment.
Bill’s Story
For many patients, the path to an accurate diagnosis is anything but simple. Take Bill, for example. At 60 years old, he had been living with neck pain for nearly a decade, often worse on the right side. Along with the pain came frequent headaches—mild ones once or twice a week and more severe episodes a few times each month. On top of that, he struggled with dizziness, a nagging sense of imbalance, and frequent “brain fog” that left him feeling less sharp than he used to.
When he first sought help, Bill was told he had BPPV (Benign Paroxysmal Positional Vertigo), a common inner ear disorder. Yet repeated Epley maneuvers, the standard treatment for BPPV, gave him no relief. Next, he was referred to vestibular therapy, but the exercises only worsened his headaches. Despite multiple evaluations, no one had considered his neck as the source of the problem.
Only later, after careful assessment of his cervical spine, did the real picture come into focus: his headaches, dizziness, and imbalance were tied to long-standing dysfunction in his neck. Once his treatment plan targeted his cervical strength and mobility, he finally began to improve. In fact, after only five visits of physical therapy, Bill reported that his headaches and dizziness had already decreased by about 80%.
Bill’s story isn’t unique. Misdiagnosis is common, and it highlights why understanding the modern concepts of cervicogenic dizziness is so important.
Modern Concepts of Cervicogenic Dizziness
Currently, the diagnosis of cervicogenic dizziness is considered a diagnosis of exclusion. A diagnosis of exclusion is a medical determination made when a specific condition is identified only after systematically ruling out other potential causes for a patient’s symptoms. This approach is commonly used when:
- Symptoms are non-specific or shared among multiple conditions (e.g., dizziness, fatigue).
- No definitive test exists for the suspected condition, requiring reliance on the absence of evidence for other diagnoses.
- Other conditions must be excluded because they present more immediate or severe risks if left untreated.
Example Conditions Diagnosed by Exclusion
- Irritable Bowel Syndrome (IBS)
- Fibromyalgia
- Chronic Fatigue Syndrome
- Cervicogenic Dizziness (CGD)
- Functional Neurological Disorders (e.g., functional seizures)
Diagnosing cervicogenic dizziness (CGD) requires a comprehensive approach, as no single test can definitively confirm its presence. Recent research emphasizes the importance of correlating dizziness symptoms with cervical spine issues while systematically excluding other potential causes. Since no single test can definitively diagnose CGD, a combination of patient history, clinical examinations, and exclusion of other conditions is essential. Let’s take a closer look at what the history of someone with cervicogenic dizziness might look like.
CHAPTER 7: Exercises To Relieve Neck Pain
Introduction
In the earlier chapters, the effects of neck pain on muscle function were discussed. Research has shown that both acute and long-term neck issues can cause fundamental changes in the way your muscles function. Over time, the deep muscles that stabilize your neck and shoulder blades can become weaker, slower to react, and even shrink in size (a process called atrophy). At the same time, the muscles closer to the surface may become overactive, trying to compensate—but not always in a helpful way.
This imbalance can lead to poor control of the head and neck, decreased endurance, and ultimately, a sense of instability. When your neck is not doing its job of stabilizing and coordinating movement, it can disrupt your body’s balance system, contributing to cervicogenic dizziness.
The good news? You can change these patterns.
This chapter is all about how to retrain and rebuild the muscles that support your neck, shoulders, and upper spine. You’ll learn simple, targeted exercises that help improve muscle coordination, postural control, and stability—without pushing through pain or doing anything complicated.
Think of this as giving your neck a fresh start. The exercises in this chapter are not about building big muscles—they’re about teaching your body how to move better and feel more stable, so your dizziness and neck symptoms begin to fade.
Whether you’ve just started noticing these issues or have been living with them for a while, these exercises are designed to meet you where you are. You don’t need special equipment or a gym—just a quiet space, a little consistency, and a willingness to reconnect with your body.
Let’s get started.
First, we need to look at some essential principles that guide the exercise approach:
- Cervicogenic dizziness exercises should start early in the rehab process.
- Exercise should not increase pain or dizziness.
- Exercises are designed to address negative changes to your muscle system.
- Precision in exercise is emphasized over speed and strength.
- Repetition is essential to improve appropriate muscle control.
The principles and neck stability exercises taught in this section are inspired by exercises from the University of Queensland, Australia. These specific motor control exercises have already been research-proven to decrease neck pain and cervicogenic headaches. Moreover, the results were maintained, boasting long-term relief (Jull et al., 2002).
Over my 24-year career, I have used these exercises to help thousands of patients with neck pain, cervicogenic headaches, and cervicogenic dizziness.
The specific exercises for rehabilitation of the muscles will be taught in two phases: motor control and strength/endurance exercises. Exercises that address position sense awareness, eye-head coordination, and balance will be taught in a different section.
Muscle System Changes
In the previous chapters, the effects of neck disorders on the muscles of the neck and shoulder blades have been described. There are also significant changes in what exercise scientists call motor control. Motor control is your body’s ability to use the right muscles at the right time to make smooth, coordinated movements.
When it comes to your neck, motor control means that the deep muscles close to your spine are doing their job—gently supporting your head, keeping it stable, and working in sync with the rest of your body. These muscles don’t create big movements; they act more like internal stabilizers, helping your head stay balanced even when you’re turning, nodding, or holding still.
However, when you have neck pain—or after an injury like whiplash or a concussion—your body can lose that natural coordination. The small stabilizing muscles may “turn off.” In contrast, the larger surface muscles like the sternocleidomastoid (SCM)orscalenes try to take over. This imbalance leads to stiffness, poor posture, muscle fatigue, and sometimes dizziness.
Motor control exercises are about retraining your brain and body to activate the right muscles again. These movements are slow, precise, and focused—not about strength or endurance at first, but about reawakening the muscles that are supposed to guide your neck.
Think of it like teaching your neck to move with grace and balance again. Before we build strength or add complexity, we first need to restore control.
Phase 1: Basic Motor Control Exercises
The first phase of the exercise program is to target the deep stabilizing muscles of the neck and shoulder blades. The exercises are low-load in nature and designed to improve the strength and endurance of the deep stabilizers. The exercises are intended to help the neck in its functional role of supporting the head against gravity. By retraining these muscles, you create a solid foundation for better posture and long-term relief from neck-related pain and dizziness.
Exercising the Deep Neck Flexors
Exercise # 1: Occipital Lift
One of the first exercises that I teach my patients in clinical practice is called the “Occipital Lift. ” This is a postural exercise that has been clinically proven to activate the deep flexor muscle group. This muscle group is essential for proper neck stability and is found to be weakened in patients who have neck pain, cervicogenic headaches, and cervicogenic dizziness.
This exercise can be performed in sitting, standing, and during dynamic activities like walking and stepper routines.

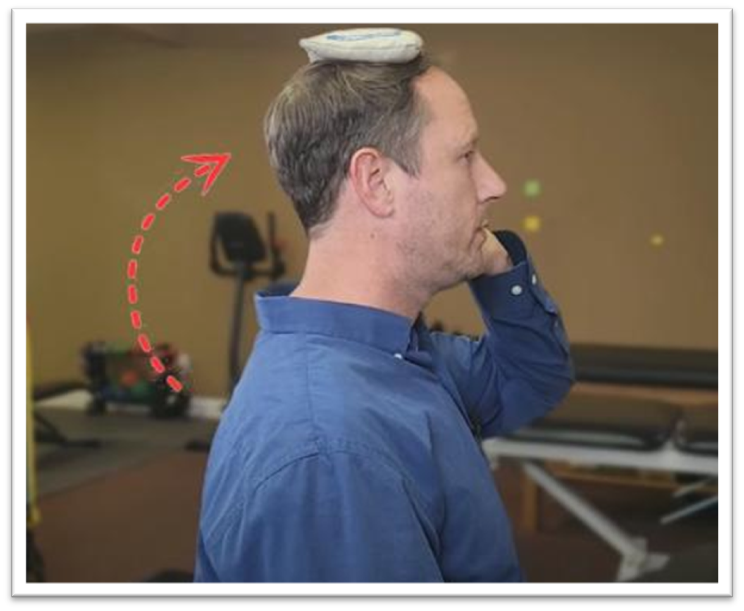
Step 1: Gently lengthen the back of your neck. This takes the weight of your head off your neck and stimulates the muscles to work. Hold the position for at least 10 seconds.
Step 2: Repeat frequently during the day (e.g., three or four times an hour). This is a gentle effort and should result in your head and neck moving into a neutral position.
Pro Tip: This exercise can be advanced by adding a small weight to the top of your head. An easy do-it-yourself project: fill a small bag with three to four oz. of rice, dry beans, beads, etc. This makes an easy weight that can be used for the occipital lift exercise.